NHS England have released new guidance on care for cancer treatment in light of the Covid-19 / coronavirus pandemic response. Many trusts and hospitals have delayed cancer treatment for two weeks whilst they evaluate and prioritise their patients. Some non-urgent care has already been delayed for 12 weeks.
Cancer treatment and the risks of coronavirus
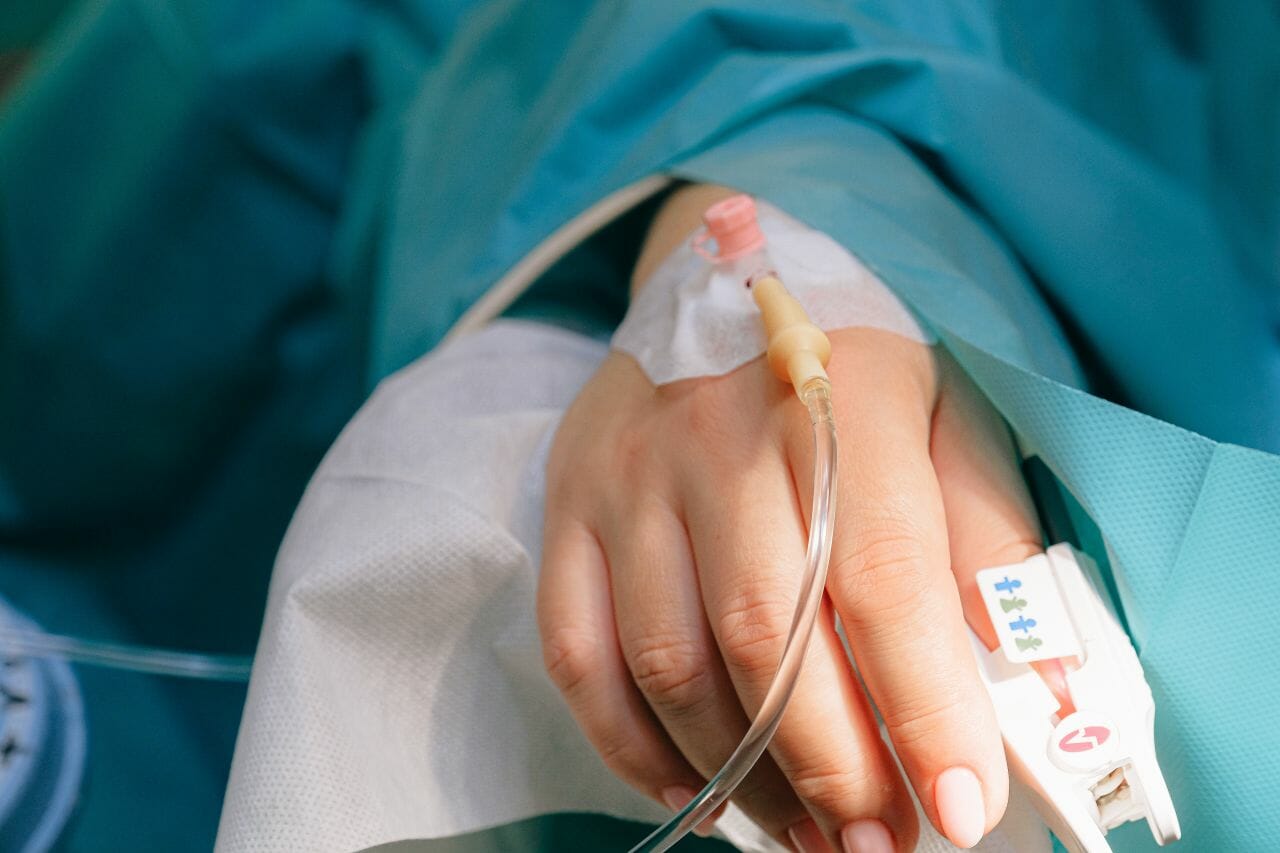
Certain types of cancer treatment can weaken the immune system, meaning that the risks of getting seriously ill with Covid-19 are increased. Those most at risk have been asked to take extra precautions and shield themselves to reduce the risk of them contracting the virus.
Hospitals and care providers are therefore having to carefully balance the risk of delaying cancer treatment versus contracting Covid-19. Attending a hospital for the life-saving treatment they need could prolong their life, but it could also increase their chances of coming into contact with Covid-19 sufferers, which if they caught it could be life threatening.
Alternative treatment or facilities
Care providers are looking at alternative ways to administer treatment, for example chemotherapy is being administered by pill to avoid patients having to come into contact with coronavirus patients.
Some private sector facilities are being commissioned to reduce the risk of cross-contamination and increase the resources available to overstretched NHS trusts. This has meant that some patients are being allowed to continue their treatment at a local private hospital which is considered ‘covid-light’ as opposed to their usual NHS facility.
Delays to treatment and diagnosis
There are patients who have had treatment delayed by 12 weeks as a result of the pandemic. NHS England has advised however that urgent treatment should still take place, so if there is an immediate risk to life, surgery and therapy should go ahead.
Cancer waiting times guidance has been changed to allow for some urgent referrals from GPs for suspected cancer to be downgraded and be sent back to GPs without diagnosis.
Priority lists
Perhaps the change that could have the most significant impact to those awaiting treatment is that cancer care providers have been asked to prepare patient priority lists in case the service becomes overwhelmed. These will help them make the extremely difficult decision of who should receive care if resources are restricted.
The emphasis has been put on curative care, with those with a strong chance of success from treatment being placed in the highest priority, over those with a low chance of survival from treatment being placed in the lowest priority. The guidelines suggest that patients should be prioritised based on the percentage of either the chance of success for curative therapy, or for adjuvant therapy the increased chance of cure to surgery or radiotherapy alone, or treatment given at relapse. Adjuvant therapy is usually a follow-on treatment for cancer, such as radiotherapy or chemotherapy after surgery.
The detail of those percentages and priority bandings are:
- Level 1: Curative therapy with a 50% chance of success or adds at least 50% chance of cure for adjuvant therapy.
- Level 2: Curative therapy with a 20-50% chance of success or adds 20-50% chance of cure for adjuvant therapy.
- Level 3: Curative therapy with a 10-20% chance of success or adds 10-20% chance of cure for adjuvant therapy, or non-curative therapy with more than 50% chance of more than one year life extension.
- Level 4: Curative therapy with less than 10% chance of success or adds less than 10% chance of cure for adjuvant therapy, or 15-50% chance of more than one year life extension.
- Level 5: Non-curative therapy with more than 50% chance of palliation/temporary control, but with less than one year life extension.
- Level 6: Non-curative therapy with 15-50% chance of palliation/temporary control and less than one year life extension.
Patient impact
Although these measures appear to be logical and most likely necessary at this time when the whole nation are being asked to make compromises to protect an already overstretched NHS, we must ask ourselves, at what cost?
Judi Rhys, Tenovus Cancer Care chief executive, said: “We know our healthcare systems are under incredible pressure, but we can’t treat coronavirus patients at the expense of looking after people living with a cancer diagnosis.”
Pryers have been helping a client claim compensation after he lost his eye as a result of a delay in his cancer being accurately diagnosed. He was due to attend another scan in March as they suspected that his cancer may have spread to his liver. This scan was unfortunately delayed due to the coronavirus. He must now wait anxiously to first, find out if the cancer has spread and then, what treatment will be available to him. He understands the strain the NHS is going through, but he also knows all too well the potential consequences of delayed treatment.
The Mirror recently reported of Carolyn’s concerns, she has secondary breast cancer and primary lung cancer. Fortunately, it is developing slowly meaning she doesn’t need to visit the hospital for treatment.
Carolyn told the Mirror; “The main worry for me during the coronavirus is the way that care is being prioritised, especially if we get to the point where there aren’t enough hospital beds.”
“If I were to get ill, I wouldn’t die from the virus I’d die from a lack of resources. If the choice was between me with an incurable illness and someone with coronavirus that was otherwise fit and healthy, I know I wouldn’t be the first pick. They would choose the person they’re most likely to save and that only really hit home when I saw the news recently were doctors had to make these decisions.”
Roisin, who was recently told that her chemotherapy would be stopped for 12 weeks, told the BBC; “It’s terrifying they’ve stopped treatment that I know is keeping me alive.”
“To have that taken away is just unbearable. How do we know it’s only going to be 12 weeks? This pandemic could go on a lot longer.”
Pryers supports the NHS in the amazing work it is doing to save the lives of those with the coronavirus. We also recognise the immensely difficult life or death decisions that the doctors have to make. It is in our view essential however, when assessing the effects of the disease, to include the cost to those that would have had treatment but for the resources having to be redirected to treat the virus.